Introduction to Evidence-Based Psychological Care
CBT vs ACT therapy are two of the most widely used, evidence-based psychological treatments available today. Both are supported by strong research for anxiety, depression, and chronic pain, but they work in meaningfully different ways. Understanding these differences is an important step toward choosing the most suitable support for your needs.
Key differences between these approaches include:
- CBT focuses on identifying and changing unhelpful thoughts, while ACT focuses on accepting thoughts and acting on personal values.
- The goal of CBT is to reduce symptoms through restructured thinking, whereas ACT aims to build psychological flexibility for valued living.
- CBT views thoughts as patterns to be questioned and tested, while ACT views them as events to be noticed without having to obey them.
- Mindfulness is a supportive tool in CBT but is central to the ACT treatment process.
- CBT is often best suited for specific symptoms and structured skill-building, while ACT can be particularly helpful for long-term conditions and values-based growth.
Both therapies are grounded in behavioural science and backed by decades of clinical research. The right fit depends on your goals, your preferences, and the challenges you are facing. For many Australians navigating mental health concerns alongside a physical alcohol dependence, the question is which approach is more likely to support change practically and sustainably.
CBT was developed by Aaron Beck in the 1960s and focuses on recognising and restructuring the distorted thought patterns that drive unhelpful behaviour. ACT was developed by Steven Hayes in the 1980s and teaches people to change how they relate to thoughts and feelings. A 2023 meta-analysis reviewing 38 studies found that both therapies produce meaningful results, with modest differences depending on the outcome measured.
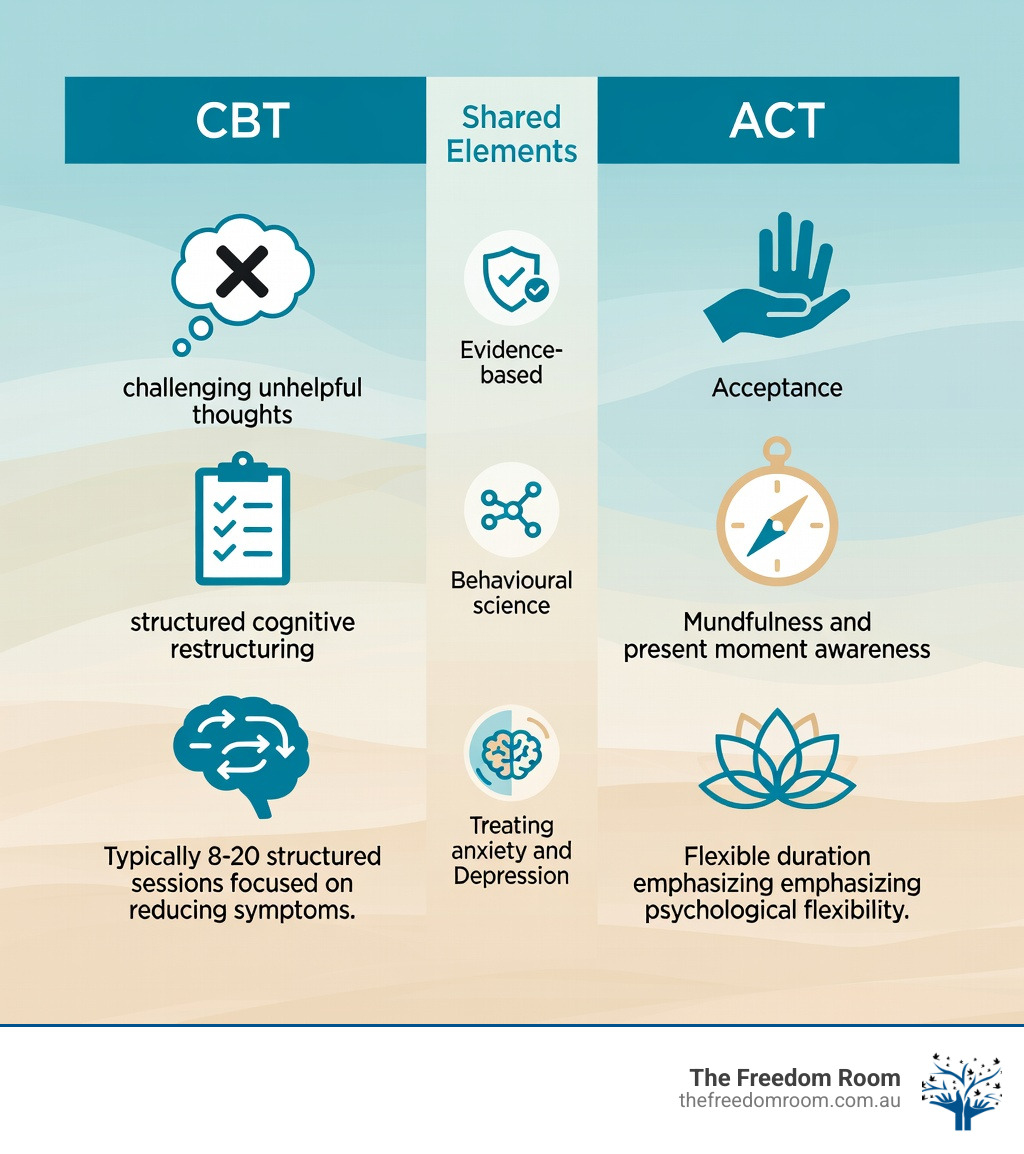
Comparing Methodologies in CBT vs ACT Therapy
The debate regarding CBT vs ACT therapy often centres on whether we should change the content of our thoughts or change our relationship with them. This philosophical divide influences every aspect of treatment, from the initial assessment to the daily exercises prescribed by a therapist. While both are considered evidence-informed treatments, their methodological paths diverge significantly.
Cognitive Behavioural Therapy operates on a corrective philosophy. It suggests that psychological distress often stems from irrational or distorted thinking patterns. By identifying these distortions and testing them against reality, a person can reduce their emotional suffering. This approach is highly effective for symptom management and has long been considered a gold standard for psychotherapy.
Acceptance and Commitment Therapy belongs to the third wave of behavioural therapies. It moves away from the idea that we must eliminate negative thoughts to be happy. Instead, it focuses on psychological flexibility, which is the ability to stay in the present moment even when thoughts are unpleasant. In this framework, the goal is not to stop feeling anxious, but to live a meaningful life while the anxiety is present.
Research highlights these nuances clearly. A three-level meta-analysis suggests that while traditional CBT often outperforms ACT in reducing specific anxiety symptoms, ACT is frequently superior in increasing mindfulness. For individuals dealing with a physical alcohol dependence, choosing between these methods often depends on whether they need structured tools to challenge triggers or strategies to accept cravings without acting on them. You can explore more about how these approaches apply to recovery through our guides on CBT for addiction and the intersection of ACT and mindfulness.
The Mechanics of Cognitive Behavioural Therapy
The foundations of CBT were laid by Aaron Beck, who observed that people with depression often experienced a stream of negative thoughts that arose spontaneously. He developed a system to help individuals step back from these thoughts and evaluate their accuracy. This process is known as cognitive restructuring.
At the heart of this methodology is the ABC model. In this model, A represents the activating event, B represents the belief or thought about that event, and C represents the consequence. CBT teaches that it is not the event itself that causes distress, but the belief we hold about it. By disputing irrational beliefs, we can change our emotional response.
Standard CBT is typically highly structured and time-limited, often spanning 8 to 20 sessions. It involves clear goal orientation and significant therapist involvement. Practitioners often use CBT techniques for addiction to help individuals identify high-risk situations and develop practical coping skills.
Common interventions used in CBT include:
- Functional analysis to identify the triggers and consequences of specific behaviours.
- Cognitive restructuring to challenge and replace unhelpful thought patterns.
- Behavioural activation to increase engagement in positive or rewarding activities.
- Exposure therapy to gradually reduce the fear associated with specific objects or situations.
- Thought records to track and evaluate the validity of negative self-talk.
- Skills training, such as assertiveness or relaxation techniques, to improve daily functioning.
The Principles of Acceptance and Commitment Therapy
ACT was developed by Steven Hayes and is rooted in Relational Frame Theory. The core premise is that suffering is a natural part of the human condition and that our attempts to control or avoid pain often lead to more suffering. The primary objective of ACT is to foster psychological flexibility.
This involves being present, opening up to experience, and doing what matters. Rather than trying to fix thoughts, ACT uses cognitive defusion to help people see thoughts as just words or images rather than absolute truths. This creates the space necessary to choose actions based on personal values rather than temporary emotions.
The ACT framework is often illustrated using the Hexaflex model, which consists of six core processes:
- Acceptance: Choosing to allow internal experiences to be present without trying to change them.
- Cognitive Defusion: Learning to observe thoughts without becoming entangled in them.
- Present Moment Awareness: Staying psychologically present and connected to the here and now.
- Self-as-Context: Recognising the part of yourself that observes your thoughts and feelings.
- Values: Clarifying what is most important to you in life.
- Committed Action: Taking concrete steps toward your values, even when it is difficult.
Comparing Outcomes for CBT vs ACT Therapy
When we look at the clinical data for CBT vs ACT therapy, the results are often comparable, but specific strengths emerge for each. For instance, research on anxiety outcomes shows that while both are effective, traditional CBT may have a slight edge in the short term for symptom reduction. In a meta-analysis, CBT outperformed ACT on anxiety with a small effect size post-treatment.
However, ACT often shows delayed gains that catch up over time. In studies of insomnia, CBT was initially superior in reducing severity, but ACT participants showed significant improvements at the six-month follow-up. This suggests that the skills learned in ACT, such as accepting discomfort, may provide a robust foundation for long-term recovery.
ACT has been shown to have a near-medium effect on improving mindfulness compared to traditional CBT. While CBT remains the gold standard for many conditions due to the volume of supporting research, ACT is proving to be an equally valid alternative. This is particularly true for those who find cognitive challenging to be frustrating or ineffective.
Integrating Mindfulness and Personal Values
One of the most significant shifts in modern psychological care is the integration of mindfulness and personal values. While traditional CBT focused primarily on the logic of thoughts, newer iterations like Mindfulness-Based Cognitive Therapy incorporate present-moment awareness to help prevent relapse in depression.
In ACT, values are the compass that guides the entire therapeutic process. Without clear values, acceptance and mindfulness can feel like passive endurance. By identifying ACT values, individuals can find the motivation to face difficult emotions or cravings. For someone in recovery, this might mean choosing to stay sober because they value being a present and reliable parent.
Mindfulness also plays a critical role in emotional regulation and mindfulness for trauma. By learning to observe the physical sensations of trauma or stress without being overwhelmed by them, individuals can build resilience. This integrated approach ensures that therapy is not just about reducing symptoms, but about building a life that feels purposeful and aligned with one’s deepest beliefs.
Ready for Change? Let’s Build a Stronger, Alcohol-Free Future Together
At The Freedom Room Wellness and Recovery, we understand that every journey toward healing is personal. Our team in Strathpine, QLD, brings a unique perspective to the table because we have lived experience with recovery ourselves. We know that the choice between CBT vs ACT therapy can feel overwhelming, but you do not have to make it alone.
We offer a compassionate and non-judgmental environment where you can explore the therapeutic path that best fits your needs. Whether you respond better to the structured, skill-building nature of CBT or the values-driven, acceptance-based approach of ACT, our goal is to provide authentic support. We combine professional expertise with genuine empathy to help you navigate the challenges of a physical alcohol dependence.
Our personalised recovery sessions are designed to be cost-effective and accessible. We believe that everyone deserves the chance to build a fulfilling, alcohol-free life. If you are ready to take that first step, we invite you to contact us today to discuss how we can walk beside you on your path to wellness.
When to Prioritise CBT vs ACT Therapy
Deciding which therapy to prioritise often comes down to your specific symptoms and how you prefer to process information. If you are someone who appreciates logic, structure, and homework tasks, you might find the direct nature of CBT very rewarding. It is particularly effective for:
- Specific phobias or panic disorders where exposure and cognitive reframing are essential.
- Severe depression where behavioural activation can provide a necessary jump start.
- Obsessive-Compulsive Disorder (OCD) using exposure and response prevention.
- Short-term goals where rapid symptom reduction is the primary focus.
On the other hand, you might prioritise ACT interventions if you have tried challenging your thoughts and found that they only seem to get louder. ACT is often the preferred choice for:
- Chronic pain or long-term health conditions where the goal is to improve quality of life despite symptoms.
- Generalised anxiety where worrying about the worry is a major factor.
- Personal growth and life transitions where clarifying values is more important than fixing a specific problem.
- Situations where you feel stuck in a cycle of avoiding difficult emotions.
Many modern practitioners use an integrated approach. They might use CBT tools to help you manage immediate triggers while using ACT principles to help you build a meaningful long-term lifestyle. The most important factor is the therapeutic alliance, finding a professional you trust who can tailor these evidence-based methods to your unique life. You can learn more about our services to see how we integrate both approaches.
Frequently Asked Questions
How long does treatment usually last for CBT vs ACT? CBT is typically short-term and highly structured, often lasting between 8 and 20 sessions. ACT can also be delivered in a short-term format, but is frequently used as an ongoing framework for personal growth and psychological flexibility, meaning the duration can vary based on individual needs.
Can I get a Medicare rebate for these therapies in Australia? Yes, both CBT and ACT are recognised under the Better Access to Psychiatrists, Psychologists and General Practitioners through the Medicare Benefits Schedule (MBS) initiative. You will generally need a Mental Health Treatment Plan from your GP to access these rebates.
Is one therapy more successful than the other for alcohol recovery? Research indicates that both are effective. CBT is excellent for developing practical coping skills and identifying triggers, while ACT is highly effective for managing cravings through acceptance and staying committed to a sober life through values-based action.
Do I have to choose just one, or can they be combined? Many therapists use an integrated approach. For example, they might use the ABC model from CBT to help you understand a lapse, while using ACT defusion techniques to help you handle the guilt that follows. Combining methods often provides a more comprehensive toolkit for recovery.
What qualifications should I look for in a therapist? In Australia, you should look for a therapist who is registered with the Australian Health Practitioner Regulation Agency (AHPRA). Many psychologists, social workers, and counsellors receive specific training in both CBT and ACT as part of their professional development.
How do I know if therapy is working? Success in CBT is often measured by a reduction in specific symptoms, like fewer panic attacks or improved mood. In ACT, success is often measured by an increase in psychological flexibility and an improved ability to engage in activities that align with your values, even if some symptoms remain.
Are there high dropout rates for these therapies? Meta-analyses show no significant difference in dropout rates between CBT vs ACT therapy. Both are generally well-tolerated, though some people find the homework in CBT or the emotional opening up in ACT to be challenging at first.

