Why Mental Health Relapse Prevention Strategies Are Essential for Lasting Recovery
Mental health relapse prevention strategies are crucial tools that help individuals maintain their recovery progress and prevent a return to previous symptoms or behaviours. Understanding these strategies is fundamental to achieving sustained wellbeing over temporary setbacks.
Key Mental Health Relapse Prevention Strategies:
- Early Warning Sign Recognition – Identifying subtle mood changes, sleep disruptions, and social withdrawal before symptoms escalate
- Trigger Management – Avoiding or preparing for high-risk situations like stress, conflict, or isolation
- Healthy Coping Mechanisms – Using mindfulness, deep breathing, journaling, and Emotional Freedom Techniques (EFT) to manage difficult emotions
- Strong Support Systems – Maintaining connections with family, friends, therapists, and peer support groups
- Lifestyle Foundations – Prioritising balanced nutrition, regular exercise, and quality sleep for emotional stability
- Professional Support – Knowing when to seek help and having a crisis plan ready
- Treatment Adherence – Staying consistent with therapy appointments and prescribed medications
Understanding Relapse in Recovery
The path to mental health recovery is often non-linear. Research indicates that approximately 50% of people with depression experience relapse after one episode, with rates increasing to 70% after two episodes and 90% after three or more episodes.
It is important to understand that relapse does not signify failure; rather, it can be an integral part of the recovery process, offering opportunities for learning and strategic adjustment.
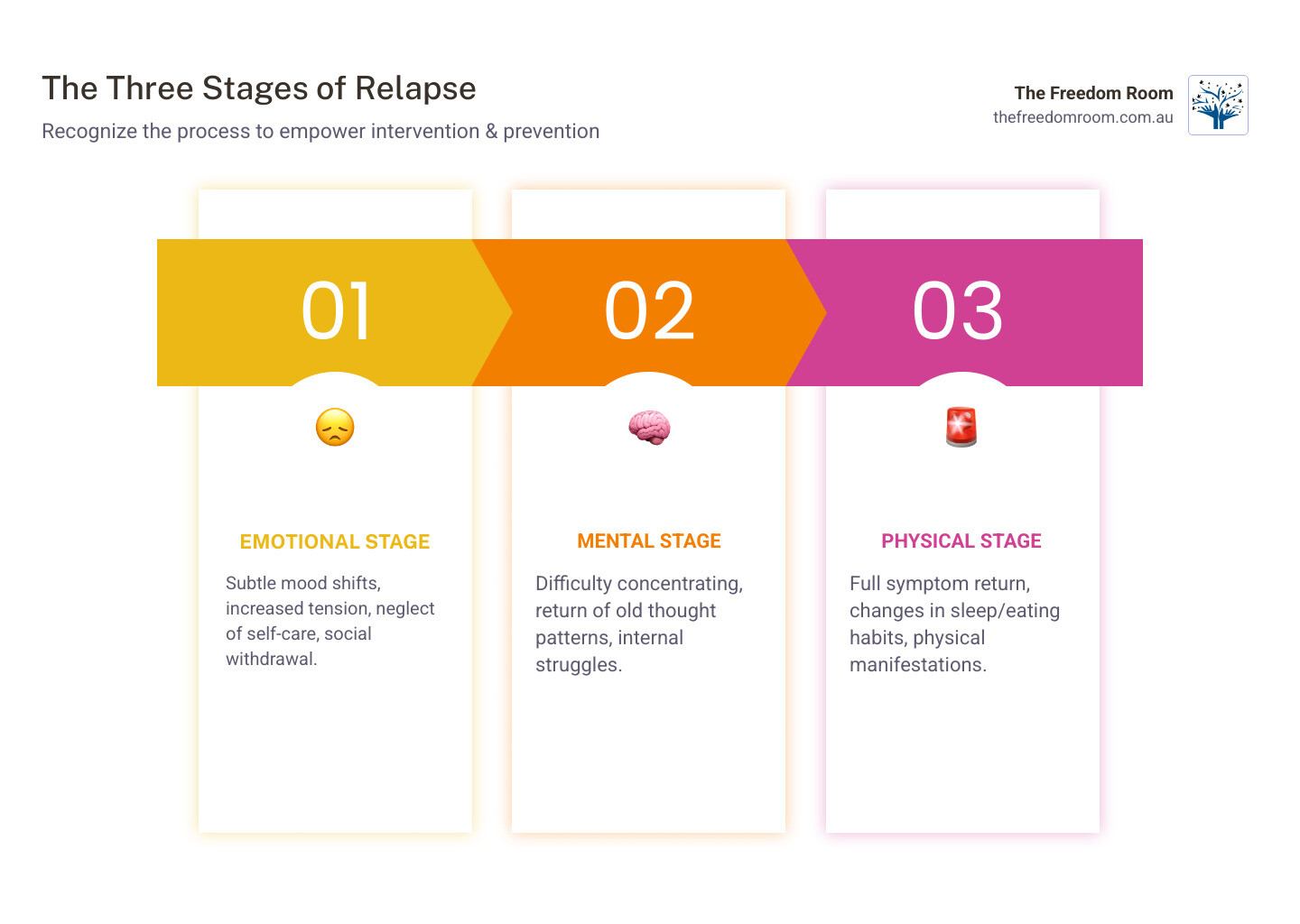
Relapse typically unfolds in three distinct stages: emotional, mental, and physical. Recognising these stages early creates opportunities for intervention before symptoms fully return. With proper planning and support, individuals can develop personalised strategies that build resilience and maintain their mental health progress.
Proactive planning forms the foundation of successful long-term recovery, empowering individuals to take charge of their wellbeing rather than simply reacting to crises.
Mental health relapse prevention strategies vocabulary:
Understanding the Nature of Mental Health Relapse
Mental health relapse represents a return of symptoms after a period of stability. A relapse does not indicate failure or that a treatment protocol is ineffective. Rather, mental health conditions are similar to chronic physical conditions like diabetes or asthma, with periods of remission and flare-ups.
The brain’s chemistry and neural pathways can be altered by mental health conditions, creating ongoing vulnerability during recovery. This biological reality makes mental health relapse prevention strategies essential for maintaining long-term wellbeing.
Statistics underscore the importance of preventative measures. For individuals with depression, approximately 50% experience relapse after their first episode. This risk increases to 70% after two episodes and reaches 90% for those who have had three or more. Similarly, around 40% of patients with schizophrenia experience relapse within the first year following hospital discharge.
These figures highlight the importance of proactive planning and ongoing support.
Viewing Relapse as a Process, Not an Event
Understanding relapse as a gradual process, not a sudden event, opens up opportunities for early intervention. The journey typically unfolds through emotional, mental, and physical stages, each offering different warning signs.
This perspective transforms how recovery is approached. Instead of waiting for a crisis, individuals can learn to recognise subtle shifts and respond before symptoms fully return. Each setback provides valuable information about what needs adjustment in a recovery approach.
The recovery paradigm offers a model of hope and change that emphasises growth, learning, and adaptation throughout the journey.
Common Early Warning Signs
The body and mind frequently provide subtle signals before a full relapse occurs. Recognising these early indicators allows for timely intervention and course correction.
Emotional and Mood Indicators
Mood shifts often appear first; an individual might notice increased irritability, persistent sadness, or unusual agitation. Increased tension or a general sense of unease can signal that the stress response system is becoming overwhelmed.
Behavioural Changes
Social withdrawal frequently follows, as maintaining relationships begins to feel overwhelming. An individual might decline invitations or avoid calls from friends and family. Neglecting self-care becomes noticeable when basic tasks like personal hygiene, preparing nutritious meals, or regular exercise start to feel burdensome.
Physical and Cognitive Symptoms
Changes in sleep patterns—whether insomnia, oversleeping, or erratic schedules—often accompany other warning signs. Changes in eating habits can manifest as significant increases or decreases in appetite, or gravitating towards less nourishing comfort foods. Difficulty concentrating makes it challenging to focus on work, follow conversations, or remember information.
Psychological Patterns
Perhaps most significantly, the return of old thought patterns signals that familiar negative thinking cycles are re-emerging. This might include harsh self-criticism, catastrophic thinking, or obsessive worry patterns from previous difficult periods.
Primary Triggers and High-Risk Situations

Triggers are specific situations, emotions, or circumstances that increase vulnerability to relapse. These can be internal triggers like certain thoughts or emotions, or external triggers such as particular people, places, or events.
Common External Triggers
Stress is one of the most common triggers, whether from work, relationships, or finances. When coping resources are overwhelmed, susceptibility to symptom return increases. Conflict in relationships can be particularly challenging, especially unresolved interpersonal tensions. Anniversaries of traumatic events can unexpectedly trigger emotional responses, bringing back painful memories or creating anticipatory anxiety.
Common Internal and Lifestyle Triggers
Lack of quality sleep significantly impacts emotional regulation and cognitive function. Poor sleep hygiene or chronic sleep deprivation can quickly destabilise mental health progress. Similarly, poor nutrition affects brain chemistry and energy levels, making it harder to maintain emotional stability. Isolation creates vulnerability, as disconnection from supportive relationships removes crucial protective factors. Substance use, including occasional alcohol consumption, can interfere with medications and disrupt the brain’s chemical balance.
Identifying Personal Risk Factors
Identifying high-risk situations requires honest self-reflection about environments where an individual feels most vulnerable. This might include social gatherings with alcohol, spending time with unsupportive individuals, or returning to places associated with past difficulties.
Proactive identification and planning significantly reduce their potential impact on the recovery journey.
Core Mental Health Relapse Prevention Strategies
Effective mental health relapse prevention strategies require a proactive and personalised approach. The goal is to establish a strong foundation of support and skills before challenges arise. This involves equipping individuals with the necessary tools and knowledge to navigate difficult periods.
The Central Role of Treatment Adherence
Adhering to established treatment plans is the cornerstone of successful prevention. This means taking prescribed medications consistently and maintaining regular therapy appointments, even when feeling well. It is a common misconception to discontinue treatment upon feeling better; however, this is often a critical time when ongoing support is most needed to maintain stability. Medication and therapy provide the foundation that supports continued stability.
The Importance of Building Resilience
Building resilience is equally crucial. Resilience is the ability to adapt and recover from life’s challenges. This involves viewing setbacks as temporary and understanding that difficulties do not define an individual’s worth or future.
Past experiences often influence present challenges. For more information on healing from these experiences, explore a trauma-informed approach.
Developing Healthy Coping Mechanisms
Developing a diverse range of healthy coping mechanisms provides a selection of tools to utilise when stress or triggers arise, rather than feeling overwhelmed.

Stress Management and Mindfulness
Stress management techniques help identify and respond to stress constructively before it becomes overwhelming. This might involve recognising physical tension, racing thoughts, or changes in breathing. Mindfulness and meditation offer powerful ways to anchor oneself in the present, helping to observe thoughts and feelings without becoming overwhelmed by them. Research, including studies on Mindfulness-Based Relapse Prevention for Substance Use Disorders, demonstrates their effectiveness.
Somatic and Expressive Techniques
Emotional Freedom Techniques (EFT), or tapping, provides a method for processing difficult emotions. This technique involves tapping on specific acupressure points while focusing on distressing thoughts, which sends calming signals to the amygdala—the brain’s alarm system—helping to disrupt the stress response. Deep breathing exercises offer immediate relief during stressful moments. Simple techniques like diaphragmatic breathing can quickly calm the nervous system. Journaling provides a private space to process emotions and identify patterns, which can help with gaining clarity, tracking progress, and recognising triggers before they escalate.
The key is finding what works for the individual. Experimenting with different approaches is important. A comprehensive Addiction Coping Skills Ultimate Guide offers additional strategies to explore.
The Importance of a Strong Support System
Recovery is seldom achieved in isolation. A strong support system is essential for preventing relapse and maintaining long-term wellbeing.
Components of a Support Network
A support network provides accountability, emotional guidance, and practical assistance. Crucially, it helps reduce the isolation that often precedes relapse. Friends and family who understand the recovery journey can offer encouragement, though this may require education and boundary setting. Therapists and counsellors provide professional expertise and objective perspectives, helping to develop new strategies and adjust the approach as needs change. Peer support groups offer connection with others who have shared experiences, which can reduce feelings of isolation and provide practical insights.
Effective Communication
Learning to communicate needs clearly to a support network ensures they can provide the most helpful assistance. This might mean explaining what support is most beneficial or being direct when experiencing difficulties.
Our Mental Health Support Complete Guide provides detailed information about building and maintaining these crucial relationships.
When and How to Seek Professional Help
Recognising when self-management strategies require professional support is a crucial skill in mental health relapse prevention strategies. Acknowledging the need for additional help is an important component of self-awareness and effective self-management.
Indicators for Professional Intervention
Escalating warning signs are a clear indication that professional support is needed. If usual warning signs are persisting, intensifying, or interfering with daily functioning, it is time to reach out. If usual coping mechanisms are no longer effective, this signals the current approach may need adjustment. Thoughts of self-harm or harming others require immediate professional attention, as they indicate a level of emotional distress where professional intervention is necessary for safety. Struggling with treatment adherence—such as missing therapy or forgetting medications—often indicates underlying issues that professional support can help address.
Types of Professional Support
Professional support comes in various forms. Psychotherapy and counselling can help process underlying issues and develop new coping skills. EFT Practitioners offer specialised support for processing emotional trauma and unresolved feelings. A medication review with a GP or psychiatrist can determine if current medications need adjustment. Creating a crisis plan with a professional ensures there are clear steps and contacts for a mental health emergency.
Seeking professional help is a demonstration of commitment to one’s recovery. The goal is to build a comprehensive support system that includes both personal relationships and professional expertise.
Building a Sustainable Recovery Lifestyle
A sustainable recovery lifestyle is built on consistency and structure rather than perfection. Mental health relapse prevention strategies are most effective when integrated into a daily routine, creating a foundation that provides support through both calm and challenging times.
Establishing predictable routines and healthy habits fosters a sense of control and stability, which reduces the likelihood of being overwhelmed by challenges. The focus should be on long-term progress. If deviations from the routine occur, the priority is to return to the established structure without undue self-criticism. Each consistent action contributes to overall recovery.

The Role of Diet, Exercise, and Sleep
The connection between physical and mental health is well-established, and daily lifestyle choices directly impact mental resilience. Nourishing the body, engaging in regular physical activity, and prioritising sleep create an internal environment that supports emotional stability.
- Balanced nutrition significantly impacts mental wellbeing. Food choices influence brain chemistry, energy levels, and mood. Whole grains, fresh fruits and vegetables, lean proteins, and healthy fats support optimal brain function. Conversely, processed foods, excessive sugar, or skipping meals can exacerbate symptoms of anxiety and depression.
- Regular physical activity is a powerful tool for managing stress and low mood. Movement releases endorphins, which are natural mood elevators. Exercise also helps process stress hormones, improves sleep quality, and builds self-efficacy.
- Prioritising sleep is a crucial aspect of mental health maintenance. Quality sleep allows the brain to process emotions and consolidate memories. When sleep is compromised, managing stress and maintaining emotional balance becomes more difficult. A consistent sleep schedule and a relaxing bedtime routine can dramatically improve mental resilience.
You can learn more about how lifestyle factors impact recovery through resources like the Better Health Channel.
Developing Personalised Mental Health Relapse Prevention Strategies
A personalised relapse prevention plan serves as a structured guide for an individual’s recovery. This is a dynamic document that should evolve as one learns more about their personal needs and effective strategies.
Step 1: Identify Warning Signs and Triggers
Begin by honestly identifying personal warning signs—the subtle shifts in mood, behaviour, or thinking that signal potential difficulties. These early indicators provide an opportunity to intervene before symptoms escalate. Next, list specific triggers, both internal (thoughts, emotions) and external (people, places, situations). Understanding these triggers enables an individual to either avoid them or prepare specific strategies to manage them.
Step 2: Outline Coping Strategies
For each warning sign and trigger, outline specific coping strategies that will be used. This might include contacting a support person, practising deep breathing, engaging in physical activity, or using EFT tapping. Having these strategies documented removes ambiguity when feeling overwhelmed.
Step 3: Establish a Support Network List
Create a comprehensive contact list including trusted friends, family, a therapist, and support group contacts. It is also critical to establish emergency contacts—such as mental health crisis lines or a GP—for urgent situations.
Step 4: Regular Review and Updates
Remember to review and update the plan regularly, especially after challenging periods or significant life changes. The plan should reflect an individual’s growing self-awareness. For detailed guidance on creating an effective plan, explore this Relapse Prevention Strategy resource.
This written plan empowers an individual to respond thoughtfully rather than reactively, providing concrete steps to follow when clear thinking is difficult.
Frequently Asked Questions about Relapse Prevention
This section addresses frequently asked questions regarding mental health relapse prevention strategies.
How does relapse prevention for mental health differ from substance use?
While substance use recovery often centres on abstinence, mental health relapse prevention strategies focus on symptom management, building stress resilience, and fostering overall wellbeing.
Rather than a separate programme, mental health relapse prevention is integrated into an ongoing treatment plan. The goal is not necessarily avoiding a specific substance, but maintaining emotional stability and preventing the return of symptoms like depressive episodes or anxiety attacks. This approach emphasises robust coping mechanisms, medication consistency, and a balanced lifestyle.
How can I support a loved one in their relapse prevention?
Supporting a loved one in their mental health recovery can be a significant role. The following actions can make a profound difference:
- Educate yourself about their specific condition, triggers, and warning signs. Understanding their experience helps you respond with empathy.
- Offer non-judgemental support by creating a safe space for them to share their struggles without fear of criticism. Active listening is often the most powerful form of support.
- Encourage professional help when warning signs are observed. Gentle suggestions are typically more effective than demands. If you are aware of their relapse prevention plan, you can assist them in adhering to their chosen strategies.
- Respect their boundaries, acknowledging that recovery is a personal process. They may require space or have specific needs that differ from what one might assume would be helpful.
What is the first step in creating a relapse prevention plan?
The first step in creating a relapse prevention plan is developing self-awareness. This involves the honest identification of personal early warning signs and triggers.
The process requires objective reflection on past experiences to understand the factors that contributed to previous difficulties. The goal is not to assign blame but to gather essential information that will inform future prevention strategies.
This initial introspection creates the foundation upon which all other prevention strategies are built. With this self-awareness, an individual can begin building the personalised strategies and support systems that will serve them throughout their recovery.
Conclusion: The Importance of Proactive Relapse Prevention
Recovery is a continuous process of building a life of purpose and wellbeing. Mental health relapse prevention strategies are not merely clinical tools but essential components of this journey, enabling individuals to manage their health proactively.
The journey is unique to each person, and seeking support is a sign of commitment to one’s health. Professional guidance, combined with evidence-based strategies, provides a robust framework for navigating the complexities of recovery.
Setbacks can be reframed as opportunities to refine strategies and strengthen resilience. Each challenge offers a chance to deepen self-understanding and enhance one’s capacity for positive change.
Sustained wellbeing is achievable with the right support and personalised strategies. For individuals seeking to develop a comprehensive plan for long-term success, professional assistance is recommended. To learn more about structured approaches, explore addiction relapse prevention strategies and discover how a personalised plan can support a successful recovery journey.

